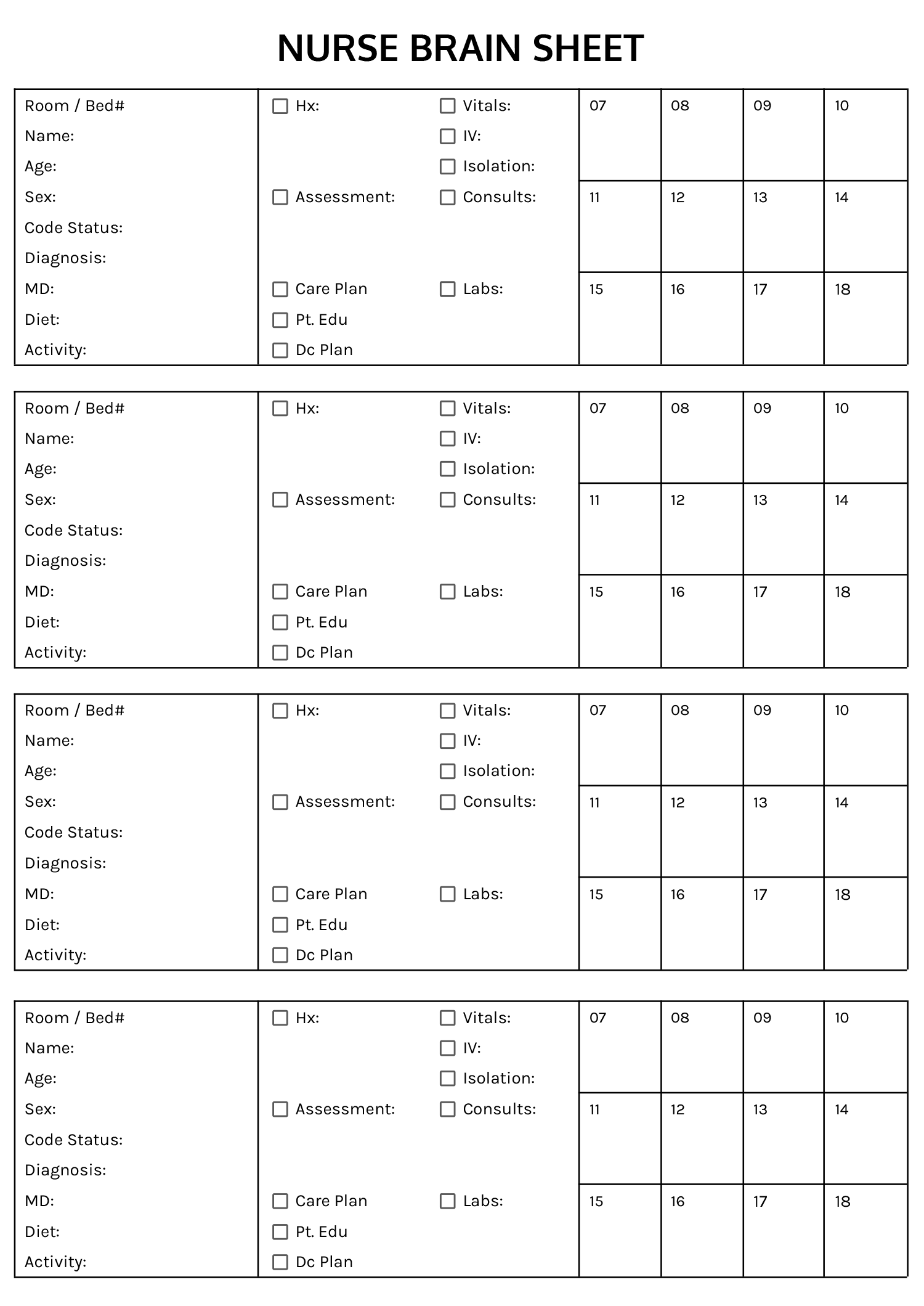
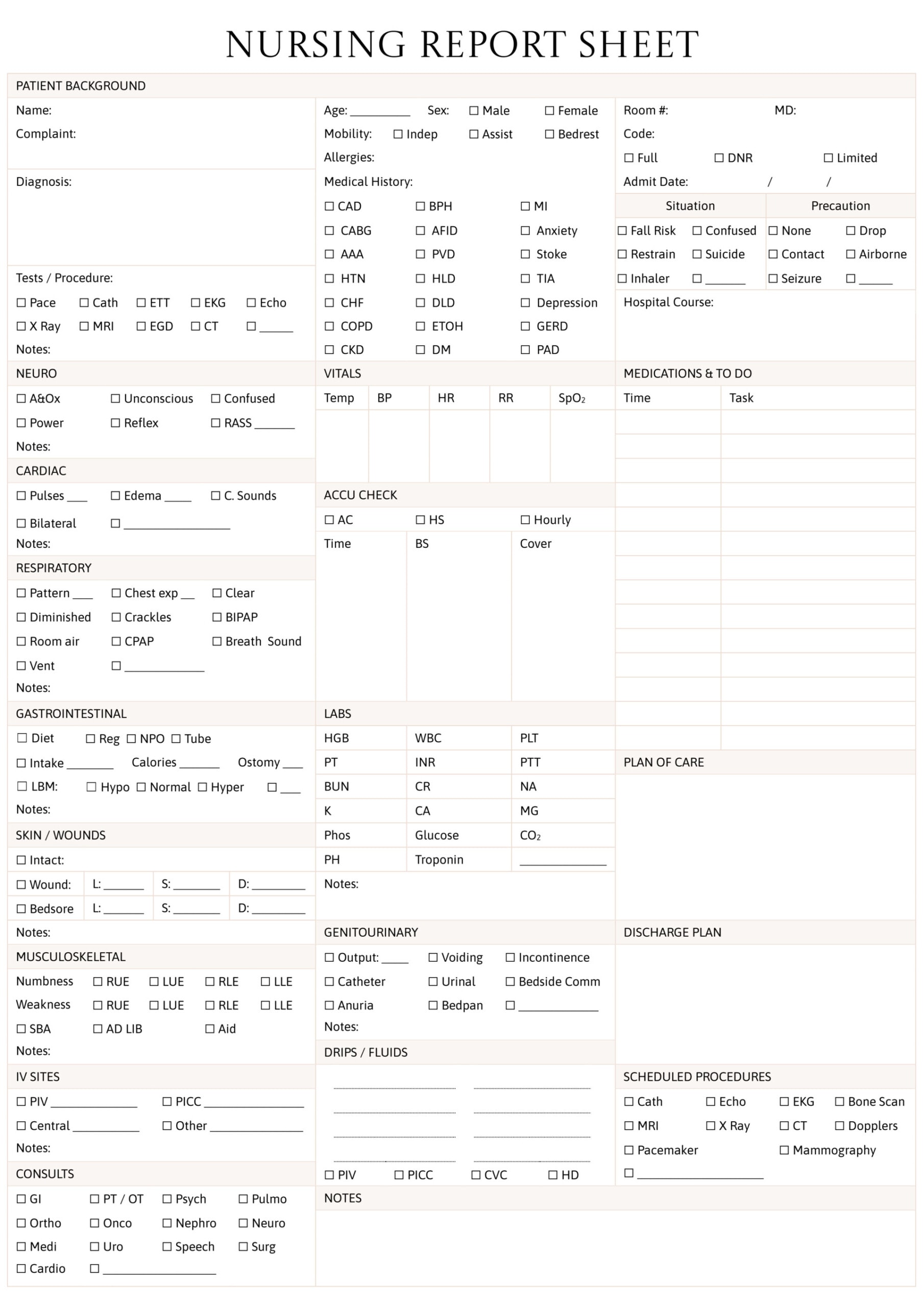
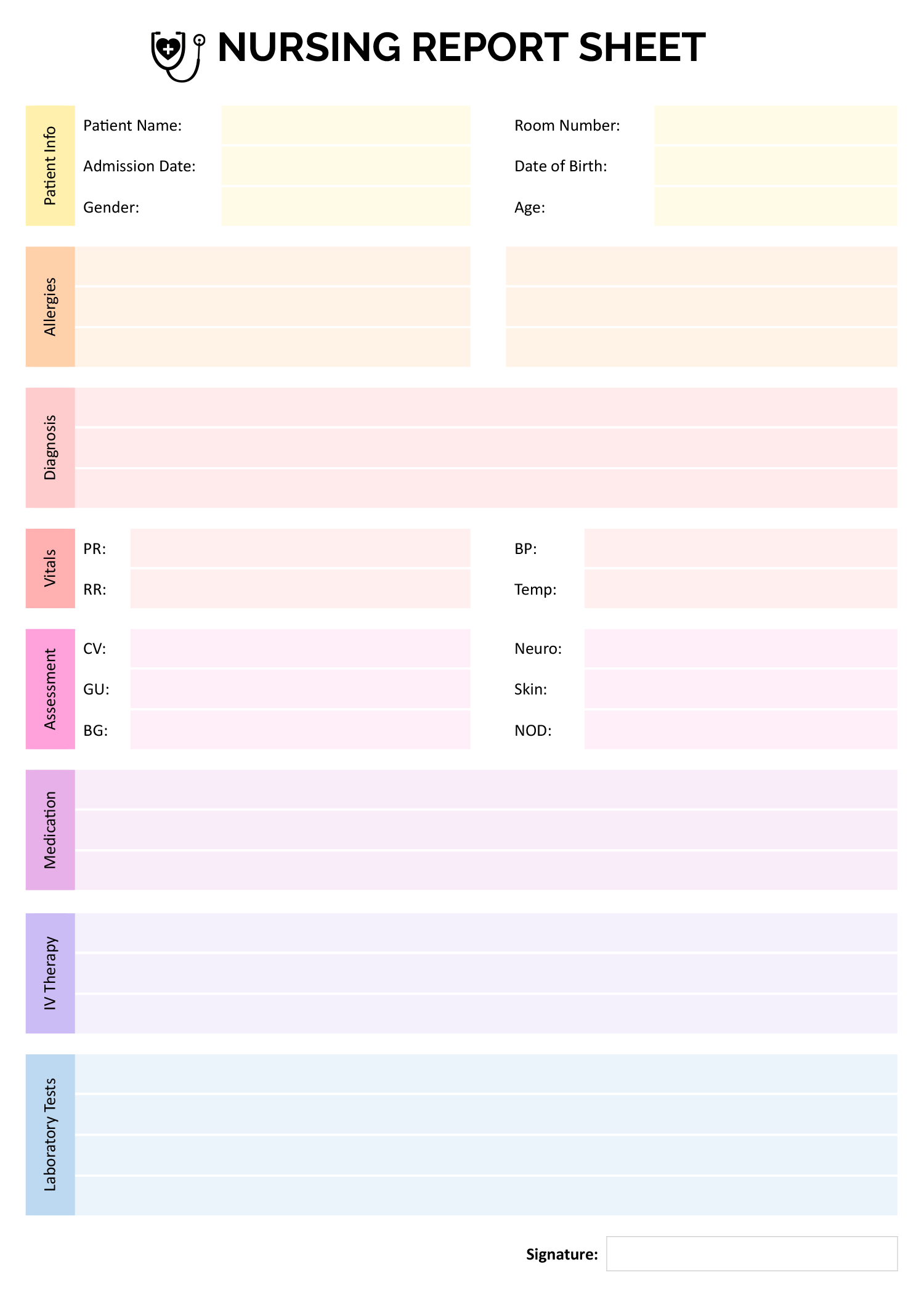
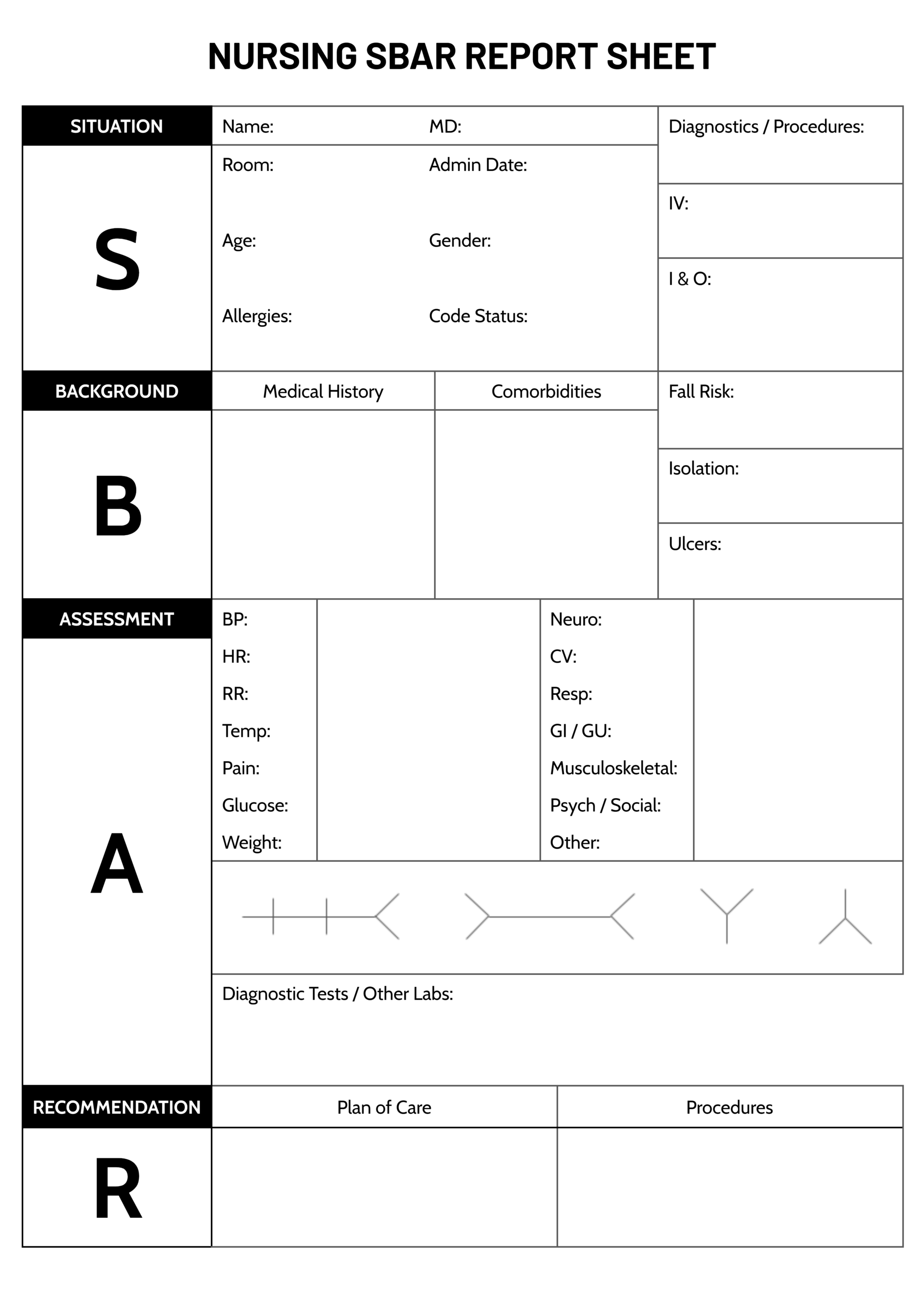
This nursing SOAP note example includes sample data in each section to show how to document patient information using the subjective, objective, assessment, and plan format. It is intended as a reference for writing clinical notes, with content covering symptoms, observations, diagnosis, and care plan. It is available in Word, PDF and Google Docs formats.